- What is patient intake?
- Why a streamlined intake process matters
- Traditional vs. digital intake: What's changed?
- What patients expect in modern healthcare
- What happens when intake works
- Intake and staffing: Doing more with less
- 5 ways to improve your intake process
- What to look for in a patient intake solution
- Intake is the first step toward a smoother workday
- Frequently asked questions about patient intake
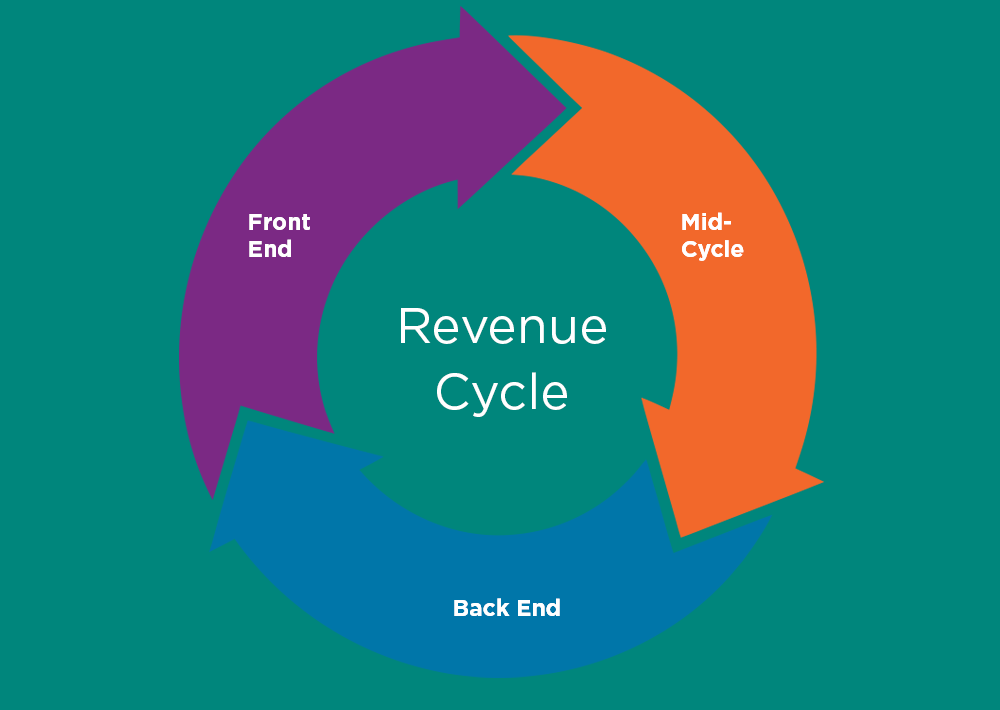
It’s Monday morning. Patients are lining up, your phone hasn’t stopped ringing and there’s a growing pile of paper forms waiting to be scanned. For healthcare organizations, the patient intake process is often a bottleneck that creates daily frustration.
Registration is one of the most time-consuming and error-prone parts of the care process. Whether you’re responsible for patient registration, payment collection or medical record updates, how you handle intake can impact everything—from claim accuracy to patient satisfaction.
In this guide, we’ll walk through what patient registration means today, what it used to look like and how modernizing it can improve your workflows, reduce administrative stress and increase collections.
What is patient intake?
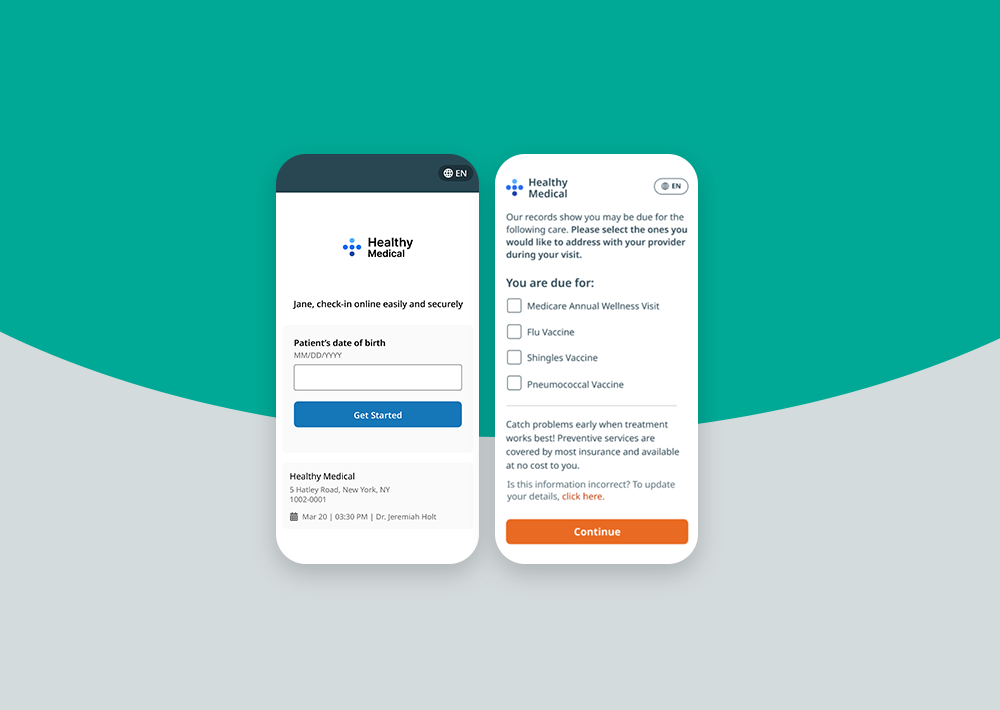
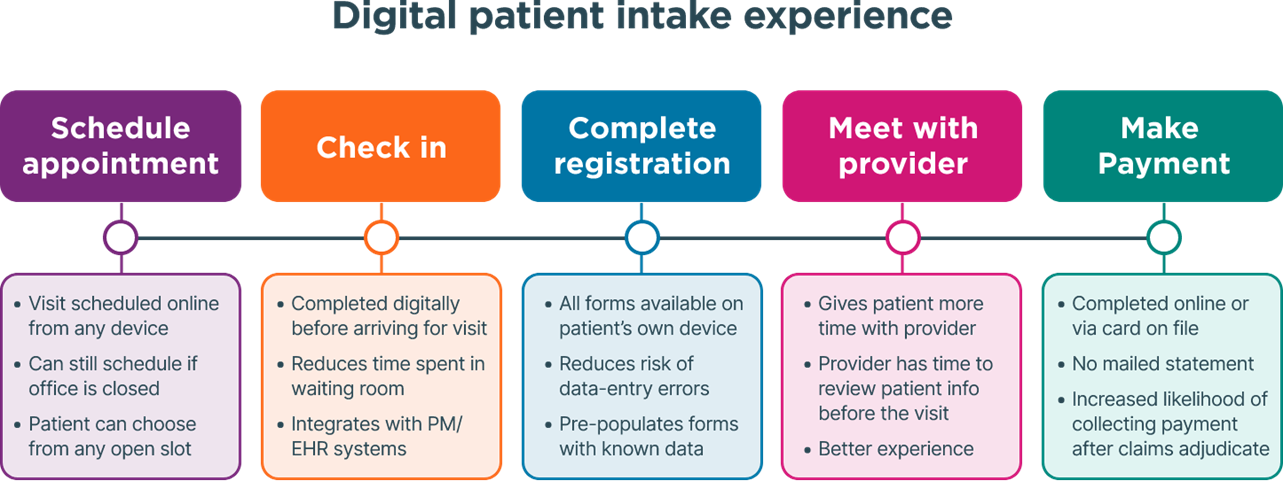
Patient intake is the process of collecting key demographic, clinical and financial information from patients before their visit. This includes:
- Name, date of birth and contact information
- Insurance details and eligibility
- Medical and family history
- Social determinants of health (SDOH)
- Consent forms and disclosures
- Preferred pharmacy and communication method
- Copayments or outstanding balances
These details help ensure accurate charting, clean claims and successful billing—but they also contribute to a positive first impression by reducing wait times, minimizing repetitive questions and helping patients feel confident that their information is correct. The result is a smoother, more efficient experience from check-in to checkout.
Digital intake simplifies your workflow
Why a streamlined intake process matters
For operational staff, patient registration sets the tone for everything that follows. A well-designed check-in process can:
- Reduce front-desk workload and save time by automating forms and insurance verification
- Improve payment collections by collecting balances upfront, decreasing bad debt
- Minimize claim errors and denials with clean, complete data that supports faster reimbursement
- Enhance satisfaction for patients with a modern, convenient experience
- Lower wait times for patients who check in ahead of time
Intake is no longer just a paperwork formality—it’s a key driver of reimbursements and revenue.
Find inefficiencies and quick wins with our 2-minute checklist.
Traditional vs. digital intake: What’s changed?
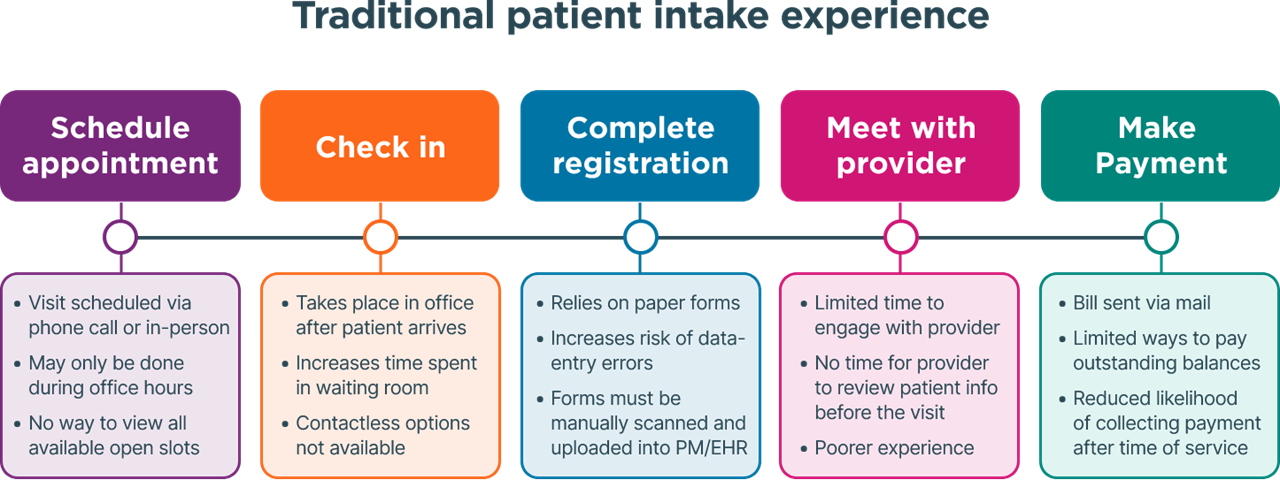
Traditional intake: familiar but flawed
In many organizations, registration is still a largely manual process. While many have moved away from fully paper-based systems, a hybrid approach is still common—where digital tools may be used for some tasks and paper forms are still relied upon for consents, questionnaires or specialty-specific documentation.
This often includes:
- Paper clipboards and printed forms
- Staff manually entering data into the EHR
- Manual insurance lookups and front-desk copay collection
While this method may be familiar, it’s also labor-intensive. It increases the risk of data entry errors, contributes to staff burnout and creates workflow bottlenecks that impact both patients and staff.
Digital intake: designed for efficiency
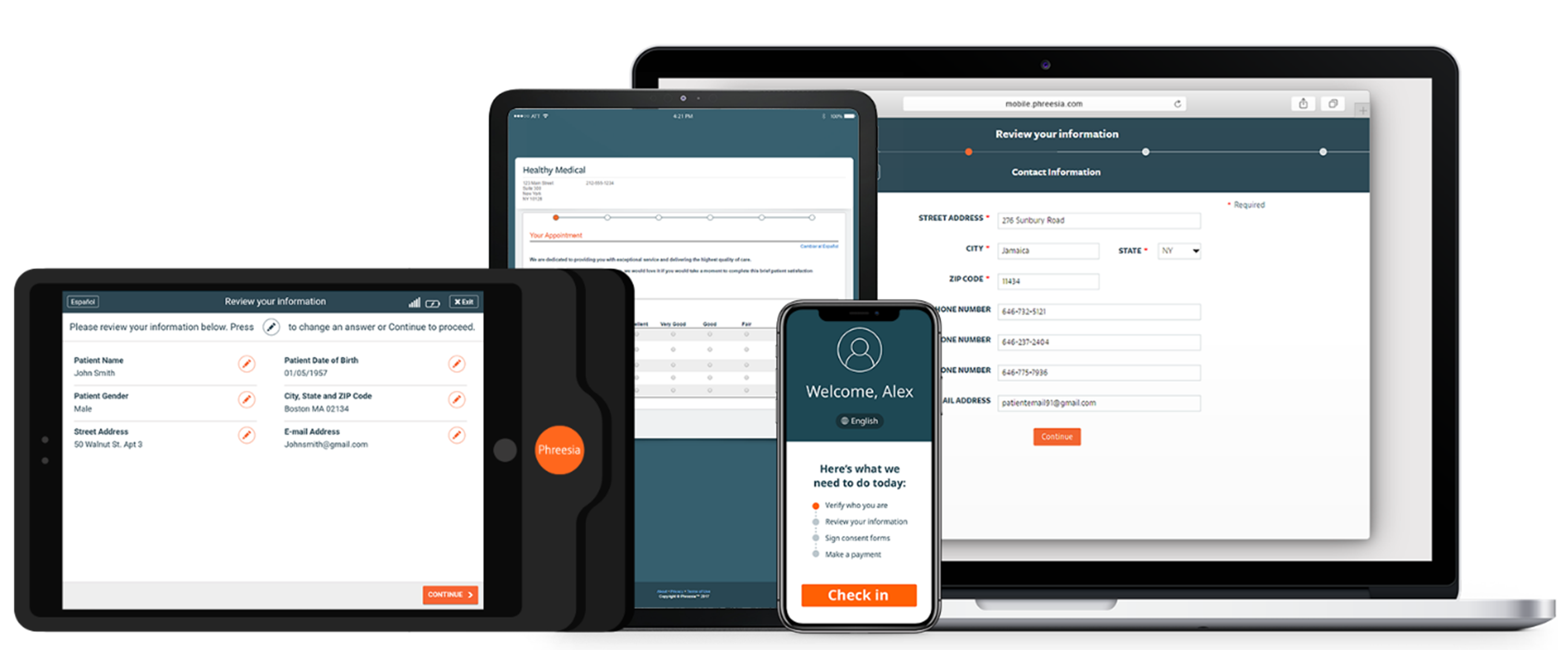
Digital registration transforms these steps into a seamless, pre-visit workflow.
Patients can:
- Complete forms and upload documents
- Verify insurance coverage
- Sign consent forms
- Pay balances
- Choose their preferred language and pharmacy
For front-desk staff, this means less manual entry, fewer delays and more time to focus on patient needs. For billing professionals, it means more complete records and faster payments.
What patients expect in modern healthcare
Today’s patients expect convenience. They’ve grown used to mobile check-ins, online forms and self-service tools in every part of their lives—from travel and banking to retail and education.
In healthcare, they’re looking for the same:
- Ease of use: Patients want to complete forms before arriving and limit time spent in the waiting room
- Transparency: Being able to review insurance details and payments up front, confirming cost accuracy
- Privacy: Secure, HIPAA-compliant platforms feel safer than paper forms
Meeting these expectations not only improves satisfaction—it reduces the pressure on your staff.
What happens when intake works
Modernizing the check-in process isn’t just a tech upgrade—it drives real results for busy operational teams.
Healthcare organizations using Phreesia have achieved:
- 3 in 4 patients pay their copay at the time of service
- Save 8 minutes of staff time per patient who self-schedules
- 3x increase in time-of-service collection rates when using Phreesia vs. staff
- 97% of patients are satisfied with their Phreesia experience
Want to see more results?
Intake and staffing: Doing more with less
Across the industry, healthcare organizations are navigating persistent staffing challenges. For front-desk and billing teams already stretched thin, manual intake only adds to the burden.
Digital registration helps lighten the load by:
- Automating repetitive tasks like data entry and insurance capture
- Reducing inbound calls by letting patients complete tasks independently
- Improving staff retention by eliminating daily inefficiencies
It’s about equipping your team with the tools they need to work more efficiently, reduce errors and deliver a better experience for every patient.
Explore a mobile-friendly check-in
5 ways to improve your intake process
Looking to streamline intake without overhauling your entire workflow?
Start here:
- Integrate registration with EHR and billing systems
Sync data directly to your systems to avoid duplicate entry and improve accuracy. - Customize workflows by patient profile
Tailor questions based on visit type, demographics or new vs. returning patient status—no more asking a teenager about Medicare. - Digitize forms and consent collection
Capture signatures electronically, avoid scanning paper and ensure all forms are stored securely. - Enable mobile pre-visit check-in
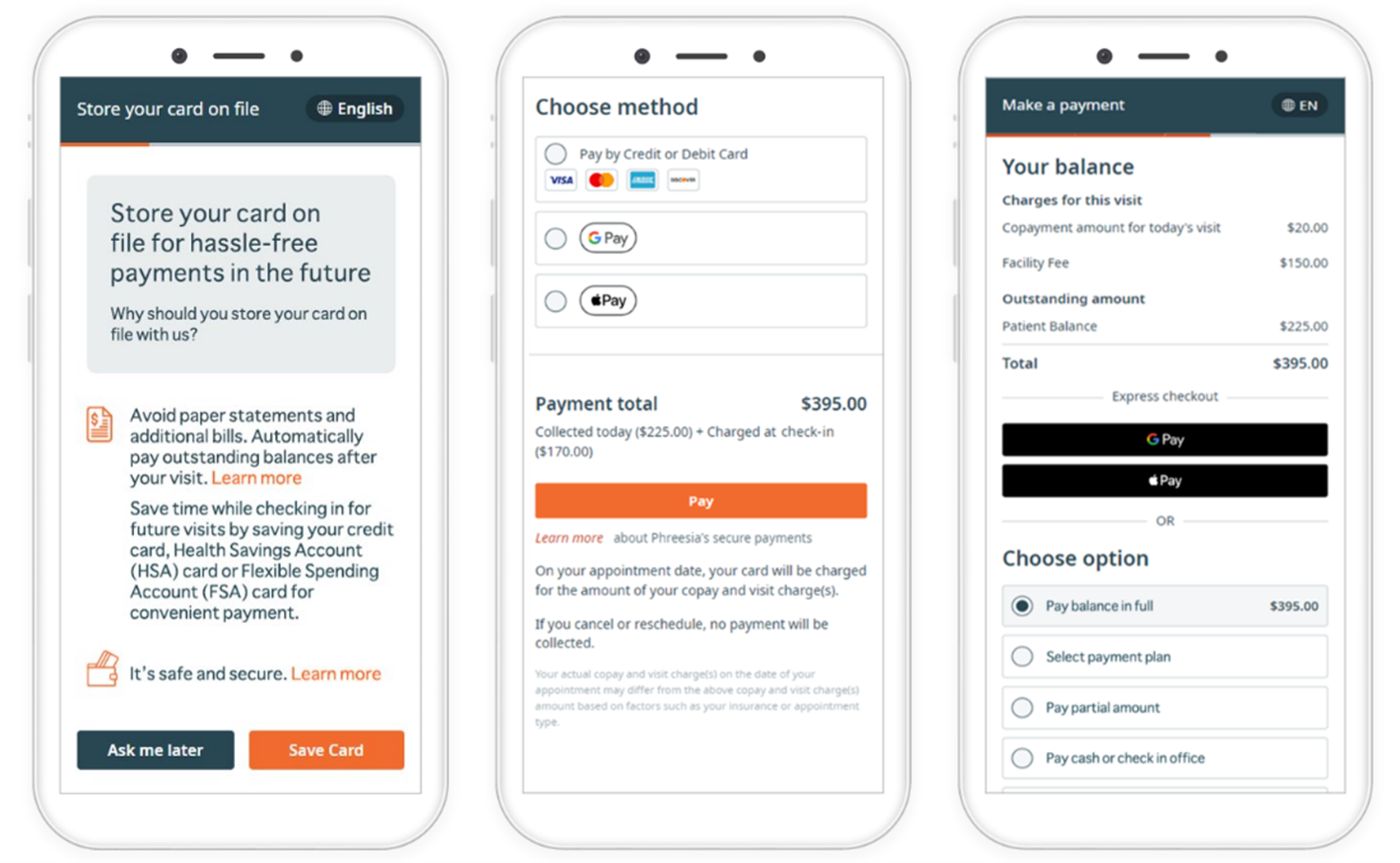
Let patients check in from home or their phone. This reduces front-desk traffic and speeds up the visit. - Collect payments at the time of service
Add secure payment prompts during intake to reduce aging A/R and simplify collections.
What to look for in a patient intake solution
Choosing the right intake software can improve your team’s workflow, but not all solutions are created equal. Here’s a simple checklist of features to help you make the right choice—whether you’re at the front desk, billing, or managing operations.
| Feature | Why it matters |
|---|---|
| Mobile check-in and digital forms | Lets patients complete check-in tasks before their visit, which reduces front-desk bottlenecks, shortens wait times and enhances patient satisfaction. |
| EHR and PM integration | Prevents duplicate data entry by syncing information directly with your existing systems, which improves billing accuracy and reduces manual workload. |
| Eligibility and benefits verification | Confirms patients’ coverage in real time, reducing the risk of claim denials, surprise bills and time spent on follow-up. |
| Customizable workflows | Allows organizations to tailor forms and questions based on visit type or specialty, ensuring patients are asked only what is relevant and reducing confusion. |
| Upfront payment collection | Enables practices to collect copays or outstanding balances before the visit, helping reduce bad debt, improve cash flow and eliminate end-of-visit delays. |
| Multilingual support | Expands access by offering forms in over 20 languages, helping non-English-speaking patients understand and complete documentation accurately. |
| Digital signature capture | Speeds up form completion by allowing patients to sign consent forms electronically, eliminating the need for printing, scanning or filing paper forms. |
| Real-time analytics and reporting | Tracks form completion rates, payment collections and staff workload metrics, enabling continuous improvement and data-driven decisions. |
| HIPAA compliance | Ensures patient data is protected throughout the registration process, helping your organization meet legal requirements and avoid costly breaches. |
| Automation of repeatable tasks | Reduces staff burden by handling repetitive tasks—like data entry and insurance checks—so teams can focus on high-touch, value-added interactions. |
Pro tip: Look for platforms that let you automate intake across the entire patient journey, from pre-visit check-in through payment and satisfaction surveys—all in one place.
A modern registration platform should not only reduce your manual workload but also help you meet your team’s financial and operational goals.

Intake is the first step toward a smoother workday
When you streamline patient check-in, wait times drop, patients are more satisfied and your billing process becomes more accurate and efficient.
Phreesia’s intake management solution is designed specifically for healthcare organizations like yours. With mobile check-in, automated data capture, real-time payment options and seamless integrations, we help operational teams like yours spend less time chasing paperwork—and more time focusing on what matters.
Learn how Phreesia helps healthcare organizations provide a modern, individualized patient intake experience—at scale.

Frequently asked questions about patient intake
What are the main steps in patient intake?
Typically, intake includes collecting patient demographics, verifying insurance, gathering medical histories, securing consent forms and collecting payments.
Why is digital registration better than paper forms?
Digital intake reduces manual work, lowers error rates, improves revenue cycle management and offers patients a more convenient experience.
How does intake affect the billing process?
Accurate, complete registration data ensures cleaner claims, fewer denials and faster reimbursement. It also makes upfront collections easier.
Can older or less tech-savvy patients still complete digital intake?
Yes—user-friendly platforms like Phreesia support accessible design, mobile optimization and in-office digital options like tablets or kiosks.