What is patient activation and why does it matter?
Patient activation is the ability of individuals to manage their own health and actively participate in their healthcare. When patients are more activated, they tend to achieve better health outcomes and contribute to improved healthcare efficiency. Here’s why patient activation is essential and how healthcare organizations can foster it.
What’s patient activation?
At its core, patient activation answers one critical question: Does this patient have the knowledge, skills and confidence to manage their health and healthcare?
While high-quality medical care is vital, patient behavior significantly impacts health outcomes. Activated patients actively participate in their care, ensuring they take medications, attend appointments and understand their financial responsibilities.
Yet, given the complexity of the healthcare system, many patients need support to become effective self-managers of their health. The goal of patient activation is to empower individuals to take independent, proactive actions to maintain and improve their well-being.
Why is patient activation important?
Research shows that activated patients:
- Are more likely to engage in preventive care and self-management behaviors
- Maintain positive habits over time
- Experience better health outcomes, lower costs and improved care experiences
For healthcare organizations, patient activation improves clinical outcomes, reduces avoidable care costs and improves performance in value-based care (VBC) arrangements. Activated patients are more likely to:
- Show up for appointments
- Follow referrals
- Avoid unnecessary emergency room visits
By equipping patients with the right tools and resources, providers can improve community health while benefiting operationally and financially.

10 strategies to increase patient activation
1. Embrace patient segmentation
Just as every patient needs a tailored treatment plan, they also need personalized approaches to care delivery. Patients’ self-management abilities exist on a spectrum:
- Less activated patients may need more guidance and support
- Highly activated patients are better equipped to self-manage
Effective segmentation involves identifying patients who are most likely to use avoidable, costly care and allocating resources where they’re needed most. For instance, providers can focus high-touch interventions on patients with high clinical risk and low activation levels.
A 2014 study highlighted the importance of segmentation in understanding population subgroups. It found that segmentation provides greater insights into patient risk than demographic or clinical factors alone, helping providers better meet the unique clinical and behavioral needs of each patient group.
2. Use digital outreach tools
Patients with low activation often struggle with preventive care, medication adherence and care transitions. Digital tools like automated text messages and calls can:
- Remind patients to schedule preventive screenings or refill prescriptions
- Encourage healthy behaviors and self-monitoring
- Reduce gaps in care and prevent unnecessary emergency visits
In a recent study by JAMA Network Open, researchers found that patients with low activation were more than twice as likely to have unplanned healthcare utilization at 30-day post-discharge than patients with high activation. Those patients also had higher rates of avoidable ED visits, which suggests their clinical needs “could have potentially been managed in a different setting.”
But by using digital outreach tools in the right ways, providers could help patients avoid unnecessary readmissions.
Automated text messages and phone calls can help increase patient activation by reminding patients to self-monitor their health, refill their prescriptions or even schedule preventive care or referral appointments. These tools enable patients to better understand their needs and practice healthy behaviors, making them more likely to seek out health information and understand the treatment guidelines for their condition.
Using outreach to increase patient activation can mitigate gaps in care, too. When patients delay preventive screenings, they’re at higher risk of experiencing negative outcomes—or even developing or exacerbating chronic diseases. As activation increases, patients are more likely to stay up to date with routine care. The end result is less time spent in the ED, fewer unexpected costs and better health outcomes overall.
3. Administer the patient activation measure® (PAM®)
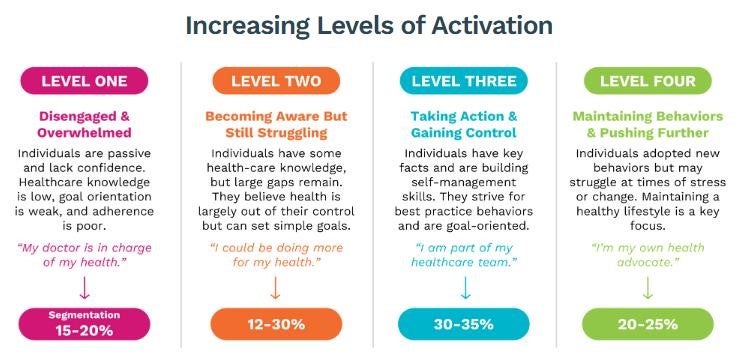
Without a reliable way to assess patient activation levels, providers may struggle to meaningfully engage patients in their care. The Patient Activation Measure (PAM) is a validated survey that segments patients into four activation levels along a 100-point scale.
PAM helps providers:
- Identify risk: Recognize patients with low activation levels that may otherwise be missed by traditional risk models.
- Tailor support: Customize education and coaching to meet patients where they are.
- Measure impact: Track improvements in patient activation over time.
Research shows that as activation levels increase, patients are more likely to develop self-management skills and achieve better health outcomes.
More than 750 peer-reviewed journal articles highlight PAM as a key variable. Patient self-management improves significantly as patient activation increases. Additionally, PAM Performance Measure (PAM-PM) is a Consensus-based entity (CBE)-endorsed performance measure (#2483).
4. Personalize patient interactions
A patient’s healthcare journey is unique, and a one-size-fits-all approach can lead to disengagement. Personalizing patient interactions ensures that communication is relevant and timely.
During the intake process, for instance, capturing a patient’s demographic data, clinical history, and PAM score enables providers to tailor conversations during appointments. This not only enhances the patient experience but also saves time for care teams.
Additionally, tools like two-way text messaging, online chats, and patient portals create opportunities for ongoing dialogue. Research backs the value of effective messaging—even for teens. In 2017, a study published in Journal of Pediatrics found that adolescents who received text-message intervention saw significant improvements in their PAM scores when compared to patients who did not receive the intervention.
Digital messaging has become even more important since the pandemic, enabling patients and care teams to have bidirectional goal-setting conversations from anywhere, even during a virtual visit. And for providers looking to deliver more patient-centered care, that’s a key value proposition. When patients can access on-demand health expertise from their mobile device or home computer, they’re more willing to proactively seek it—and less likely to delay important care.
5. Tailor education and coaching
Patients are more likely to succeed when care teams provide education and coaching that aligns with their activation level. By systematically assessing a patient’s knowledge, skills, and confidence, providers can create personalized care plans that:
- Focus on actionable steps to build confidence
- Highlight measurable goals to track progress
- Celebrate successes to reinforce positive behaviors
A study published in the American Journal of Managed Care found that coaching tailored to activation levels led to improved biometrics, better regimen adherence, and reduced hospitalizations.
6. Support patient activation with team-based care
Want to improve outcomes for your entire patient population? Get your team on board.
Too often, healthcare fragmentation is a hinderance to patient activation. Care teams can be complex— not only consisting of a patient and a clinician, but also nurses, pharmacists, support groups and dozens of other caregivers and staff members who help patients navigate care. While these stakeholders work toward shared goals, they also have vastly different approaches to patient care. And if care teams don’t communicate effectively, patient outcomes suffer.
“A team-based approach is especially important when caring for patients with complex care needs,” researchers said in a 2018 National Academy of Medicine report. “To manage the large amounts of information and multiple handoffs inherent in caring for complex patients, there is a need for seamless communication and transitions among health care professionals.”
For example, more than 35% of patients receive a specialist referral annually, yet up to 50% of referring physicians are unaware if their patient followed through. Technology that tracks referral statuses can close this gap, ensuring patients complete their care journey.
By fostering collaboration between providers, nurses, pharmacists, and support staff, organizations can emphasize each patient’s role in their care and improve outcomes across the board.
7. Provide financial assistance
For many patients, financial barriers are a significant hurdle to accessing healthcare. Even highly activated patients can face challenges navigating insurance requirements, prescription costs, and out-of-pocket expenses. Patients with lower activation levels are particularly vulnerable, as they may lack the knowledge, skills, or confidence to understand their financial options or advocate for themselves.
Financial challenges don’t just impact patients—they affect healthcare organizations, too. Patients who delay or forgo care due to cost concerns are more likely to:
- Experience acute health crises requiring expensive emergency interventions.
- Skip preventive care, leading to worse outcomes over time.
- Miss follow-up visits or fail to schedule referrals and diagnostic tests, negatively impacting revenue and value-based care (VBC) performance metrics.
To address these challenges, healthcare organizations can use technology to:
- Verify insurance and assess financial needs: By collecting accurate patient demographic and insurance information, providers can identify patients who may qualify for financial assistance, Medicaid, or sliding-scale fees.
- Offer flexible payment solutions: Payment plans or other options can help patients manage their financial responsibilities without delaying care.
- Provide proactive education: Patients can be automatically informed of their copays, deductibles, and benefits before appointments, helping them prepare financially.
Technology to enhance financial accessibility
A patient engagement tool can also alert eligible patients to specific benefits, like Medicare Annual Wellness Visits or Well Woman exams, ensuring they utilize preventive services. Additionally, healthcare organizations can:
- Identify prescription cost assistance programs: Provide educational materials about financial aid or discount programs for newly prescribed medications.
- Screen for underinsured or uninsured patients: Early identification of these patients allows organizations to connect them with affordable insurance options or community resources.
By addressing financial barriers with proactive, tech-enabled solutions, healthcare providers can ensure that cost does not prevent patients from accessing the care they need. This approach not only improves patient activation but also enhances the patient experience and strengthens financial performance for healthcare organizations.
8. Address social determinants of health (SDOH)
Social determinants of health (SDOH)—such as housing, food security, and transportation—can significantly impact patient outcomes and activation levels. Patients with unmet social needs often lack the motivation, skills, or confidence to manage their health effectively.
Research shows a reciprocal relationship between SDOH and activation:
- Higher activation can mitigate the negative impact of SDOH. For example, individuals with higher activation are more likely to access needed care and fill prescriptions, even when facing financial challenges or lack of insurance.
- Lower activation can amplify the effects of SDOH. Patients with low activation levels may delay care, miss medications, or fail to engage in preventive measures, worsening their outcomes.
In a 2021 study by Insignia Health, researchers found that pairing efforts to address SDOH with initiatives to increase activation resulted in significantly better outcomes. Another study found that individuals with high activation levels were more likely to obtain needed care and prescriptions despite being uninsured, compared to those with lower activation levels facing similar circumstances.
The takeaway? Addressing SDOH and activation together can substantially improve health outcomes and reduce disparities.
9. Reduce no-shows and gaps in care
Missed appointments and care gaps aren’t just inconvenient—they have serious consequences for patient health and healthcare organizations. Patients who frequently miss appointments often experience higher rates of emergency department (ED) visits, more hospitalizations, and poorer chronic disease management. These issues are closely linked to low patient activation.
To address this, healthcare organizations can use patient engagement tools to:
- Send appointment reminders: Automated reminders via text and phone give patients multiple opportunities to confirm or cancel visits. One study found that no-show rates dropped by 14% when patients received text reminders in addition to phone calls.
- Enable self-scheduling: Empowering patients to book their own appointments increases their engagement and responsibility for their care.
- Close care gaps: Consistent, targeted outreach emphasizes the importance of routine care and encourages patients to stay on track.
Reducing no-shows benefits all healthcare organizations by maintaining full provider schedules and improving workflow efficiency. For those in value-based care contracts, the stakes are even higher, as success depends on keeping patients healthy and preventing costly care episodes.
By actively engaging patients, providers can help them stay current with their care, avoid unnecessary costs, and improve long-term outcomes.
10. Engage patients post-visit
Engaging patients doesn’t end when their appointment does. Post-visit communication is crucial for improving activation levels and strengthening the patient-provider relationship.
Patient surveys are a valuable tool for gathering insights about patients’ thoughts, feelings, and perceptions of their care experience. This feedback provides actionable data for healthcare organizations to fine-tune their processes and improve the patient experience.
Research has shown that post-visit engagement builds confidence and improves activation. For instance:
- A guide by Ipsos MORI and The Strategy Unit found that reflective surveys helped patients feel more confident about their care, boosting their activation levels. Patient satisfaction is directly linked to activation. Organizations that use survey feedback to make meaningful changes see higher satisfaction scores and more engaged patients.
- Additionally, digital tools like secure messaging platforms allow patients to ask follow-up questions, clarify instructions, and discuss concerns from the convenience of their home. This ongoing communication makes patients feel supported and encourages them to take an active role in their health.
The result? More engaged patients, better outcomes, and stronger patient-provider relationships.

The bottom line
Patient activation is a powerful strategy to improve health outcomes, reduce costs, and enhance patient experiences. By empowering patients with the knowledge, tools, and confidence to manage their care, healthcare organizations can build healthier communities and achieve operational success.
Learn how Phreesia can help you increase patient activation, improve health outcomes and engage patients in their care.




