- Automation in healthcare: what it means for medical groups now
- Why automation in healthcare matters more now
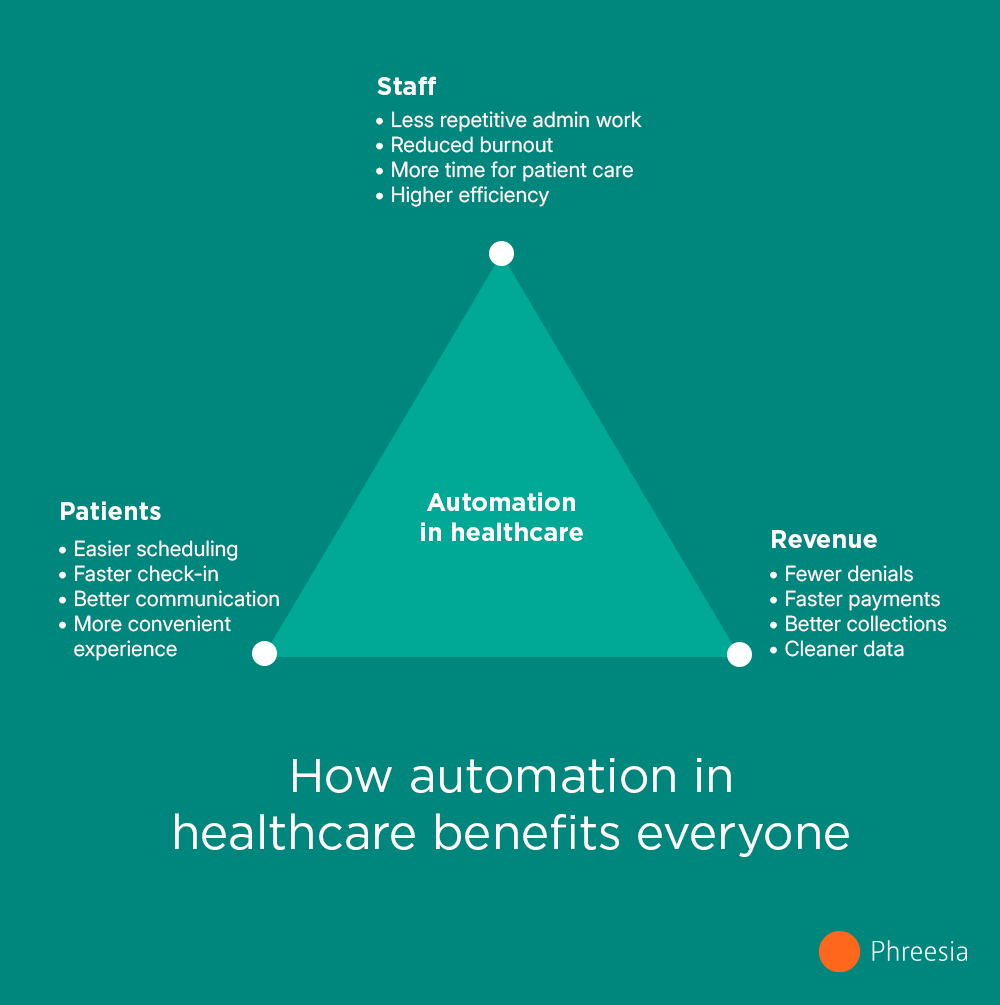
- How healthcare automation supports staff capacity and workforce sustainability
- How automation improves patient access and the patient experience
- How automation strengthens financial performance and data quality
- Where AI automation in healthcare fits into the story
- How Phreesia helps with automation in healthcare
- What medical groups should automate first
- How to implement healthcare process automation without creating new problems
- What the future of automation in healthcare looks like for medical groups
- The takeaway
- Frequently asked questions (FAQs)
- Conclusion
Author: Kathleen Ferraro | Expert review by: Chris Bays
Automation in healthcare helps medical groups take repetitive, time-consuming work off their teams’ plates so staff can focus on patients instead of paperwork. When applied to the right workflows, it can improve access, reduce errors and create a smoother experience for both patients and staff without adding complexity.
Automation in healthcare is quickly becoming a practical response to a very real challenge. Medical groups are being asked to do more with limited staff, rising patient expectations and increasingly complex administrative work. From scheduling and intake to billing and follow-up, the volume of tasks hasn’t slowed down—but the capacity to manage them manually has.
At its core, healthcare automation means using technology to handle repetitive, rules-based or high-volume tasks with less manual effort. This article breaks down 15 practical ways it can improve how medical groups operate day-to-day, including supporting staff capacity, improving the patient experience, strengthening financial performance and more.
Automation in healthcare: what it means for medical groups now
Today, automation in healthcare spans the full patient journey. It supports front-office workflows, revenue cycle processes, patient communication and day-to-day operational management.
In practice, that means automating the high-volume, repeatable tasks that traditionally rely on manual effort, like:
- Automated intake and registration
- Eligibility verification
- Appointment scheduling and reminders
- Payment collection
- Workflow tracking
It’s also worth separating automation from artificial intelligence. Most healthcare process automation today is rules-based: For example, if a patient has an appointment, send a reminder. AI automation in healthcare builds on that foundation by adding more adaptive capabilities, like conversational tools or smarter routing. But it’s still layered onto the same core workflows.
It’s also worth noting that with automation and AI alike, the goal isn’t to replace people. Instead, it’s a tool you can use to reduce friction so your staff can spend less time on repetitive tasks and more time on patient-facing or higher-value work.
Why automation in healthcare matters more now
Automation in the healthcare industry is getting more attention because the day-to-day reality for medical groups has changed. Teams are stretched thin, patients expect more and the work itself has become more complex. And those small pressures can add up quickly.
Here’s the breakdown:
- Ongoing staffing shortages and burnout: Staffing gaps and administrative overload aren’t going away anytime soon. Automation helps take repetitive work off staff plates, which can ease some of the strain that leads to burnout.
- Rising patient expectations for convenience and speed: Patients are used to managing everything from their phones, and healthcare is no exception. Without automation, keeping up with those expectations often means more manual work for staff.
- Pressure to do more without increasing costs: Medical groups are expected to improve access and responsiveness without simply adding more staff. Manual workflows in areas like scheduling, intake and billing make that hard to sustain.
- The need to recover time and reduce friction: A lot of the day is spent on small, repetitive tasks that add up. Automation helps give that time back and makes it easier for patients to move through the process without delays.
- A higher bar for operational performance: The baseline for what feels like a good experience has shifted—faster responses, fewer errors and smoother workflows. Automation is quickly becoming part of how medical groups keep up.
How healthcare automation supports staff capacity and workforce sustainability
One of the most immediate impacts of automation in healthcare is how it changes the day-to-day experience for staff. Instead of spending hours on repetitive tasks, teams can shift their time toward work that actually requires their attention.
Here’s how automation makes that happen:
- It reduces repetitive administrative work across intake, scheduling and follow-up: Automation takes on high-volume tasks like sending reminders, collecting forms and verifying information, reducing the amount of manual work staff need to manage.
- It helps relieve burnout by removing manual, low-value tasks: Repetitive, task-heavy work—like chasing paperwork or re-entering data—adds up over the day and contributes to burnout. Automating those tasks reduces administrative burden, according to Sneha Patel, MPAS, PA-C, CEO of Metroplex Medical Centres.
- It improves staff efficiency: Medical automation reduces back-and-forth communication and manual data entry. This helps front-office teams move patients through workflows more efficiently (without the need to focus on paperwork and phone tag).
- It enables staff to spend more time on higher-value responsibilities: When routine work is handled automatically, staff can shift their focus to activities that require judgment, communication and care coordination. “It lessens the administrative burden so staff can focus on the most important aspects of healthcare, including better customer service and face-to-face patient interaction,” says Patel.
- It creates a stronger case for training and role evolution: As routine, task-based work becomes automated, roles naturally shift toward responsibilities that require judgment, communication and problem-solving. That creates an opportunity to invest in training and development. This allows staff to move into more specialized, patient-facing or operational roles instead of staying focused on repetitive tasks.
How automation improves patient access and the patient experience
Automation also directly shapes how patients experience care. “Once they become acclimated to the change, patients are able to get faster, more efficient care and response from the clinical team,” says Patel.
Let’s break it all down:
- It makes it easier for patients to schedule, confirm, reschedule and prepare for visits: Automation gives patients more control over scheduling and pre-visit tasks, whether that’s booking appointments online, confirming via text or completing forms ahead of time.
- It reduces no-shows and avoidable gaps: Automated reminders and outreach help patients stay on track with appointments, reducing missed visits and keeping schedules full.
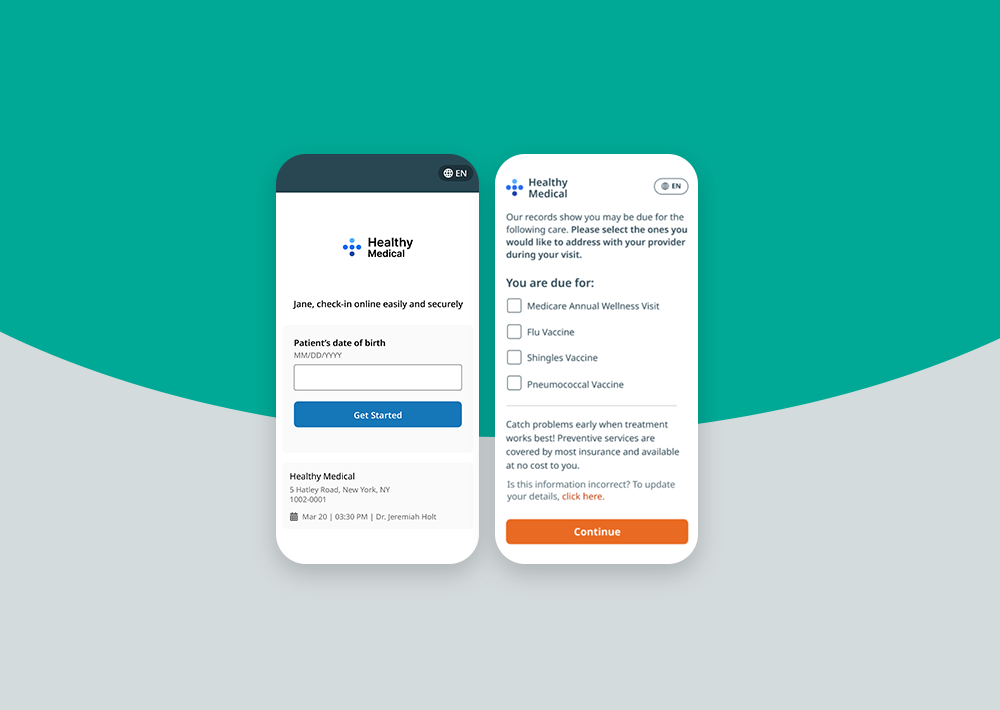
- It improves intake and registration: Digital intake moves repetitive tasks outside the waiting room. Patients can complete forms, verify information and review details before they arrive, making check-in faster and less stressful.
- It supports more personalized, timely communication at scale: Automation makes it possible to send the right messages at the right time—like reminders, instructions or follow-ups—without relying on manual outreach for every patient.
- It helps medical groups stay responsive as patient volume grows: Research shows that rising patient volume and workflow constraints can disrupt access and efficiency, making it harder for teams to keep up. Automation helps staff manage scheduling, patient communication and access without needing to increase staffing at the same pace.
How automation strengthens financial performance and data quality
Automation shows up in your financial performance and data quality, too. When information is captured more accurately and workflows run more consistently, there are fewer issues later with billing, collections and reporting.
More specifically:
- It improves data accuracy: Automation reduces the need for staff to re-enter information across systems, lowering the risk of typos, missing fields and duplicate records. More consistent data upfront supports better clinical and operational decisions.
- It supports cleaner eligibility, benefits, billing and collections workflows: Automating steps like insurance verification, payment collection and balance communication helps ensure that key financial processes happen consistently and at the right time.
- It helps reduce revenue leakage tied to missed steps, denials or incomplete information: When workflows are automated, fewer steps get skipped. That reduces the risk of denied claims, missed charges or incomplete documentation that can lead to lost revenue.
- It lowers the cost of manual work: Manual processes are time-consuming and resource-intensive. Research shows that automation is often used to replace repetitive tasks in order to improve speed, efficiency and resource utilization, which can help reduce the operational cost of routine work.
- It gives leaders more reliable operational data: Automation creates more consistent, trackable workflows, making it easier to measure performance, identify issues and make informed decisions about where to improve.
Where AI automation in healthcare fits into the story
AI automation in healthcare is often part of the same conversation as broader healthcare automation—but it plays a slightly different role. While most automation today follows clear, rules-based workflows, AI adds a layer of adaptability on top of those systems.
Instead of just executing predefined steps, AI can help interpret inputs and respond more dynamically. In practice, that can look like:
- Smarter routing of patient messages
- Conversational tools that help answer questions or guide next steps
- Systems that prioritize tasks based on urgency
That said, AI doesn’t replace the foundation. It builds on it. Without your staff’s judgement alongside well-designed workflows for intake, scheduling, communication and payments, even the most advanced tools won’t perform well. The value comes from combining reliable automation with more adaptive capabilities where they make sense.
How Phreesia helps with automation in healthcare
Phreesia puts automation to work across the entire patient journey—not just one piece of it.
Phreesia’s AI-powered platform goes beyond rules-based automation—using intelligence built on 20 years of workflow data across 4,650+ healthcare organizations to handle scheduling, intake, eligibility, payments and patient communication in one connected system.
The results are measurable: an 87% reduction in call volume, 3x more patient-reported data captured versus manual processes and 78% fewer no-shows. When automation runs end-to-end on one platform, the gains compound—cleaner intake means fewer denials, fuller schedules mean more revenue, and staff spend less time on paperwork and more time on patients.
“It lessens the administrative burden so staff can focus on the most important aspects of healthcare, including better customer service and face-to-face patient interaction.”—Phreesia customer Sneha Patel, MPAS, PA-C, CEO, Metroplex Medical Centres
What medical groups should automate first
With so many possibilities, it’s easy for automation in healthcare to feel overwhelming.
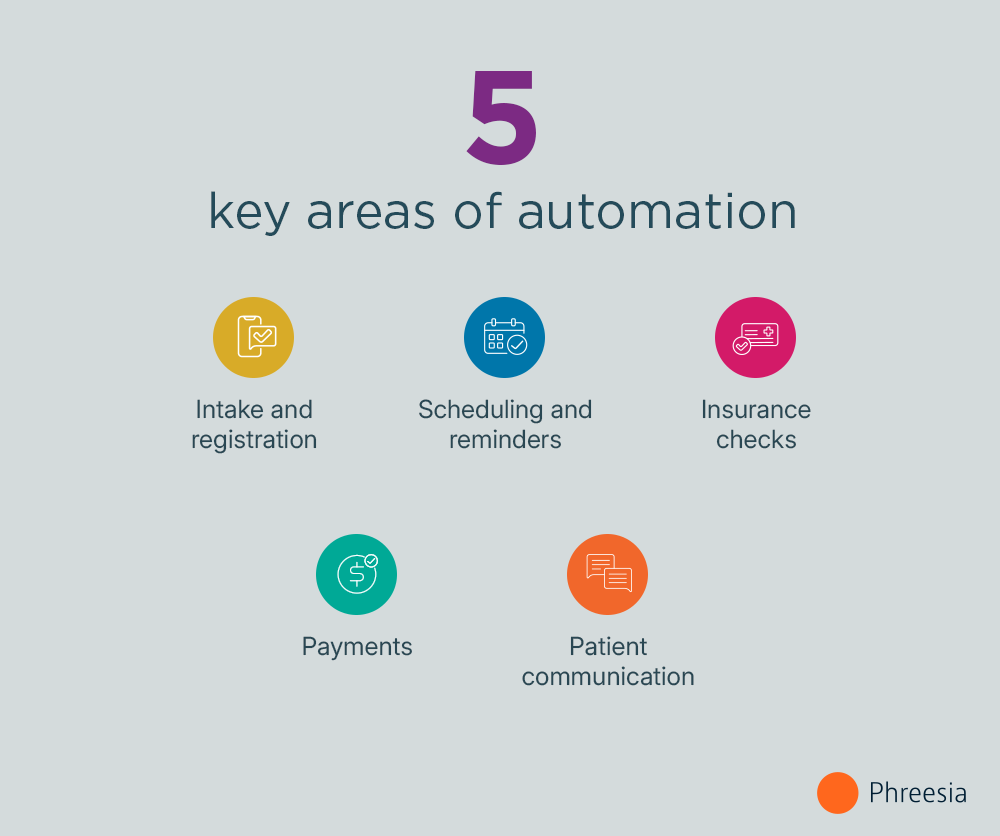
The best place to begin is with high-volume, repeatable tasks that follow clear rules, including:
- Intake and registration: Tasks like collecting patient information, forms and consents are time-consuming and highly repetitive. Automating intake helps reduce front-desk workload and improves data accuracy before the visit even begins.
- Scheduling and reminders: Appointment scheduling, confirmations and reminders are constant sources of manual work. Automating these steps improves access while reducing phone volume and no-shows.
- Insurance-related workflows: Eligibility, benefits checks and coverage validation are critical—but often manual. Automating these processes helps reduce errors and prevent downstream billing issues.
- Payments and billing touchpoints: Automating payment collection, balance notifications and receipts makes it easier for patients to pay and helps improve collections without adding staff workload.
- Patient communication workflows: From pre-visit instructions to follow-ups, communication is often fragmented. Automation helps ensure patients get timely, consistent information without relying on manual outreach.
How to implement healthcare process automation without creating new problems
Rolling out automation sounds straightforward…until it isn’t. Without the right approach, new tools can end up adding extra steps, slowing people down or creating workarounds that defeat the purpose. That’s why the ultimate goal is to make things simpler for staff.
Here’s how to do it:
- Design automation around existing workflows: Start by understanding how work actually gets done today. Automation should simplify and streamline those workflows, not force staff to adapt to rigid or disconnected systems.
- Invest in staff training and clear role definition: Adoption depends on whether staff feel confident using the new tools. Clear training, expectations and support help teams understand how automation fits into their day-to-day work.
- Focus on usability and simplicity: If a system is hard to use, staff won’t use it consistently. Prioritize tools that are intuitive and reduce effort, rather than adding new steps or complexity.
- Ensure strong integration across systems: Automation works best when systems connect. Data should flow between tools without requiring manual re-entry or workarounds.
- Measure what matters and adjust over time: Track metrics like time saved, staff satisfaction, patient engagement and operational performance. Use that data to refine workflows and improve how automation is used over time.
What the future of automation in healthcare looks like for medical groups
Automation in the healthcare industry is an ongoing shift in how medical groups operate. The biggest gains aren’t coming from individual tools, but from how those tools connect across the patient journey.
We’re already seeing that play out. Instead of isolated tasks, workflows are starting to link together. Intake connects to scheduling, scheduling to billing, and everything feeds into reporting. That makes it easier to see what’s happening in real time.
Looking ahead, automation, analytics and AI will work more closely together. Automation handles routine work. Analytics shows where things are breaking down. And AI helps teams respond to things like patient calls more quickly and intelligently.
But the human side of care doesn’t change. Staff are still essential for judgment, empathy and patient relationships. The real opportunity is using automation to create more capacity so teams have more time for the parts of care that matter most.
The takeaway
- Automation in healthcare helps medical groups reduce repetitive work, improve consistency and free up staff time for higher-value, patient-facing tasks.
- The biggest impact comes from applying automation to high-volume, repeatable workflows (like intake, scheduling, communication and payments).
- Automation improves both sides of the experience. It makes operations more efficient for staff while making care more convenient and accessible for patients.
- Financial performance and data quality benefit from more consistent workflows and more accurate information captured upfront.
- AI is expanding what automation can do, but its success still depends on strong underlying workflows and thoughtful implementation.
- The most successful medical groups use automation intentionally, starting with high-impact areas and building toward more connected, scalable operations.
Frequently asked questions (FAQs)
What is automation in healthcare?
Automation in healthcare is all about using technology to take repetitive, time-consuming tasks off your team’s plate. That can include things like patient intake, appointment scheduling, insurance checks, reminders and payments—basically the work that happens over and over again every day.
What is AI automation in healthcare?
AI automation builds on automation by making those processes a bit smarter. Instead of just following fixed rules, AI can help interpret information and respond more dynamically—like powering conversational tools or helping prioritize tasks.
How is healthcare automation different from AI automation in healthcare?
Think of healthcare automation as the foundation: It handles predictable, rules-based tasks. AI automation adds a layer on top, helping systems adapt and respond to more complex or changing situations.
What are the biggest benefits of healthcare automation for medical groups?
The biggest payoffs include less manual work for staff, smoother workflows, better patient access and communication, more accurate data and stronger financial performance.
What should medical groups automate first?
Start with the tasks that happen most often and take the most time, like intake, scheduling, reminders, insurance verification, payments and patient communication. These are usually the easiest wins and have the biggest day-to-day impact.
Conclusion
Automation in healthcare is no longer a nice-to-have for medical groups. It’s becoming a practical way to keep up with growing demands, limited staffing and higher patient expectations.
When used thoughtfully, automation helps recover time, improve consistency and make the patient experience feel more consistent and connected. The biggest impact comes from focusing on the right workflows—those repetitive, high-volume tasks that slow teams down and create friction for patients.
You don’t need to automate everything at once. Instead, apply automation where it makes the biggest difference for both staff and patients, then build from there. Done well, it gives medical groups a way to scale operations without losing the human side of care.
A version of this article was published on January 4, 2022.