- Medical check-in: what it is and why it matters now
- The modern patient check-in procedure: step-by-step workflow
- Key benefits for healthcare organizations
- Key benefits for patients
- What to look for in a medical check-in system
- How Phreesia helps with medical check-In
- How AI is changing medical check-in
- Medical check-in online: best practices for pre-registration
- On-site check-in options: kiosks, tablets and front desk workflows
- Security, privacy and compliance considerations
- Implementation playbook: how to roll out digital check-in
- Measuring success: KPIs and ROI for medical check-in
- The takeaway
- Frequently asked questions (FAQs)
- Conclusion
Author: Kathleen Ferraro | Medically reviewed by: Alicia Cowley, MD
Medical check-in is more than a front-desk task. It’s a high-impact workflow that shapes everything from patient flow to billing accuracy. When it’s designed well, it can reduce wait times, ease staff burden, and improve data quality before the visit even begins. This guide breaks down what a modern check-in looks like, why it matters and how to improve yours in practical, measurable ways.
Medical check-in has evolved far beyond a clipboard at the front desk. Today, it’s a workflow that starts before the visit and continues through arrival, verification and the handoff to care. When it’s fragmented—think paper forms, manual entry, disconnected systems—it creates delays, staff strain and data errors that carry into billing and clinical workflows.
And nowadays, patients expect to handle forms and payments from their phones. At the same time, healthcare teams face growing operational pressure. That makes check-in a key leverage point for improving patient flow, reducing staff workload, and strengthening revenue cycle performance.
In this guide, we’ll break down what modern medical check-in looks like, the benefits of improving your patient check-in procedure and how to build a better system.
Medical check-in: what it is and why it matters now
Medical check-in is the process of collecting and verifying the information needed to deliver care. It’s a series of steps that starts before a patient walks through the door and continues through arrival and the handoff to clinical teams.
That workflow usually includes:
- Confirming identity and demographics
- Verifying insurance
- Completing forms and consents
- Collecting payments
- Gathering clinical questionnaires
More and more, this happens through medical check-in online tools. That way, patients can take care of it on their own time instead of rushing through paperwork in the waiting room.
This is where things get real operationally. Check-in sets the tone for the visit. It also shapes how much pressure lands on front office staff, and determines whether clinical and billing teams are working with clean, complete information or chasing down gaps later, according to Matthew Moore, MBA, CPHIMS, CHCIO, Chief Technology Innovation Officer at Effingham Health System.
“The healthcare industry continues to shift into a technology-focused business where using new products that enhance the patient experience is key,” he explains.
When check-in runs smoothly, everything downstream feels easier. When it doesn’t, the cracks show up fast: Longer waits, frustrated patients and avoidable errors that create more work for everyone involved.
The modern patient check-in procedure: step-by-step workflow
A well-designed patient check-in procedure works a lot like a relay. Each step builds on the one before it—shifting work earlier, simplifying arrival and making it easier for staff to focus on what actually needs attention. When these pieces are aligned, check-in feels quick and predictable instead of rushed and reactive.
Here’s a step-by-step breakdown:
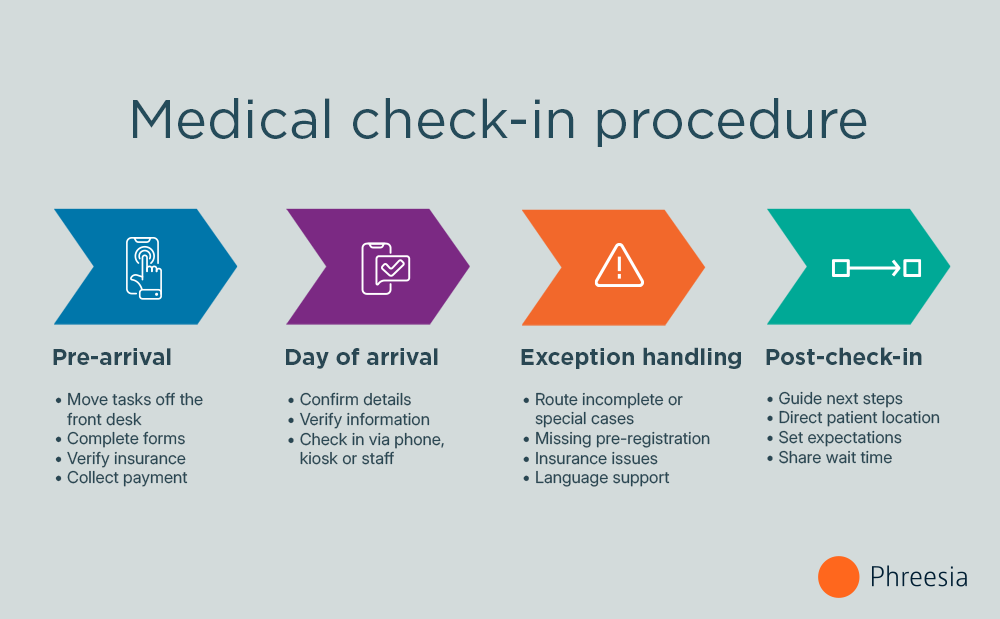
- Pre-arrival: The primary goal? Shift work off the front desk. The most effective medical check-in systems move key tasks before the visit. Patients complete forms, verify insurance and handle payments on their own time digitally. This reduces front-desk congestion and spreads the workload more evenly.
- Day of arrival: This is the time to confirm details, not start from scratch. Whether patients check in on their phone, at a kiosk or with staff, the process should be fast and focused on verification rather than data entry.
- Exception handling: It’s still important to plan for what doesn’t go smoothly. Not every patient completes pre-registration, and issues like missing insurance or language needs will come up. Clear fallback paths ensure these cases are handled efficiently without slowing down everyone else.
- Post-check-in: After check-in, patients need clear next steps—where to go, what to expect and how long they might wait. That visibility reduces confusion and helps the visit feel more organized from the start.
Key benefits for healthcare organizations
Improving medical check-in has a ripple effect across operations, staff experience and financial performance. Key benefits include:
- Increased throughput and fewer bottlenecks during peak hours: When more patients complete tasks ahead of time, arrivals move faster. Even small shifts can make a measurable difference—one study found that moving just a few minutes of data collection earlier in the process reduced patient wait times by up to 54% and improved overall flow.
- Reduced manual data entry and fewer downstream errors: Digital check-in minimizes the need for staff to re-enter information, says Moore. This reduces the risk of typos, missing fields and duplicate records. And cleaner data upfront means fewer issues later with eligibility and benefits checks, coding and billing.
- Better staff efficiency and reduced burnout: “Reliance on printing, scanning and faxing creates added burden on the staff that can be quickly alleviated by using digital check-in,” says Moore. That shift allows staff to focus on higher-value tasks and reduces the day-to-day strain that leads to burnout.
- Stronger revenue cycle performance: Accurate insurance information and upfront payment collection help reduce denials and rework. When patients understand and pay balances earlier in the process, health systems see more consistent point-of-service collections.
- More consistent, reportable processes across locations and service lines: A standardized medical check-in system creates consistency across sites, making it easier to track performance, identify gaps and scale improvements. Instead of each location handling check-in differently, teams can align around a shared workflow and set of metrics.
Key benefits for patients
Improving the patient check-in directly shapes how they experience care from the moment they arrive (or even before). Here are the primary perks:
- Faster, more convenient arrival experience: “Having to sit in the waiting room to complete paperwork prior to a visit takes away time that could be better spent with a provider,” says Moore. “Utilizing tools that allow patients to complete registration on their own time takes away the time crunch.”
- Greater transparency on forms, consents and payments: Digital check-in makes it easier for patients to see exactly what’s required ahead of time—whether that’s forms to complete or balances to pay—so there are fewer surprises at the front desk.
- Improved privacy for sensitive information: Answering questions digitally allows patients to share personal or sensitive details more comfortably than speaking out loud in a public space.
- Better accessibility and inclusivity: Multi-language options, clearer interfaces and assistive features make it easier for a wider range of patients to complete check-in independently, regardless of age, language or ability.
- More control and confidence: When patients can review instructions and complete steps ahead of time, they may feel more prepared and less rushed at arrival.

What to look for in a medical check-in system
Not all medical check-in systems are created equal. Digitizing paperwork is helpful, but the ultimate goal is to actually reduce friction for patients and staff while improving data quality.
Here’s what to prioritize:
- Multi-channel check-in options: Patients should be able to check in the way that works best for them, says Moore—whether that’s from their phone, an on-site kiosk or tablet, or with help from staff. Offering multiple pathways increases adoption and ensures no patient gets stuck.
- Real-time insurance verification and benefits checks: A strong system should be able to check patients’ eligibility and benefits at the right points in the workflow. This helps catch—and resolve—issues early.
- Flexible payments: Look for tools that support copays, outstanding balances and saved payment methods. Making it easy for patients to understand and pay what they owe upfront can improve collections without slowing down the check-in process.
- Pre-registration and forms management: The system should support sending forms in advance, with smart logic that only asks relevant questions. Features like e-signatures, reminders and the ability to upload documents help ensure forms are complete before arrival.
- Reporting and analytics: You should be able to see what’s working (and what’s not), says Moore. That includes metrics like completion rates, drop-off points, payment collection, patient satisfaction scores and operational performance across locations.
- Integration requirements: A medical check-in system should work seamlessly with your EHR and practice management systems rather than adding new layers of complexity. This is critical to “allow for quality data interchange to avoid creating duplication of work,” says Moore.
How Phreesia helps with medical check-In
Phreesia powers 1 in 6 U.S. patient visits—and medical check-in is where that scale shows up most.
Patients complete registration, verify insurance, sign consents and pay balances from their own device before they ever walk through the door. AI-driven eligibility verification helps catch coverage gaps early so they don’t become denied claims later. Smart intake forms adapt based on patient responses, so patients only answer what’s relevant—reducing drop-off and improving data quality. And when patients do arrive, staff spend 75% less time on manual data entry because Phreesia has already done the work.
The result: shorter wait times, cleaner data and more revenue collected before the visit even begins. Within 6 months of implementing Phreesia, practices see an average 73% increase in time-of-service collections. Nearly 1 in 4 denied claims traces back to a registration or eligibility error; Phreesia catches those mistakes at check-in, before they cost you. That’s why 4,650+ healthcare organizations trust Phreesia to run their check-in workflow—not just to digitize paperwork, but to make the entire process smarter.
How AI is changing medical check-in
Digital check-in was the first step in modernizing medical check-in. AI is the next one—and it’s already reshaping how the workflow runs. Where traditional check-in automation follows fixed rules (send a reminder, collect a form, verify insurance), AI adds a layer of intelligence that makes each step more adaptive and more accurate. In practice, that looks like:
- Smarter intake forms: AI-powered intake adapts in real time based on patient responses, asking follow-up questions when clinically relevant and skipping what isn’t. The result is more complete, more accurate clinical data without making the process longer for patients.
- Proactive eligibility and benefits verification: Rather than running a standard eligibility check, AI can identify coverage gaps, flag authorization requirements and surface potential denial risks before the visit—giving staff time to resolve issues instead of chasing them after the fact.
- Intelligent outreach and pre-registration nudges: AI can identify which patients are most likely to drop off before completing pre-registration and trigger targeted outreach at the right moment, improving completion rates without adding staff workload.
- Voice AI for check-in related calls: Patients who call to confirm appointments, ask about what to bring or request help with forms can be handled automatically by an AI agent. This frees staff from routine calls and ensures patients get answers immediately, 24/7.
- Continuous improvement from real-world data: Unlike rules-based systems, AI learns from patterns across thousands of interactions, improving routing, form logic and outreach timing over time. The more it runs, the better it gets.
The practices seeing the biggest gains from medical check-in aren’t just digitizing the old process. They’re using AI to make it fundamentally smarter—catching problems earlier, reducing manual work and creating a smoother experience for patients and staff alike.
Medical check-in online: best practices for pre-registration
Offering medical check-ins online only works if patients actually complete it. The key is making pre-registration simple, well-timed and easy to finish. That way, it reduces work on the day of the visit instead of shifting friction elsewhere.
Here are best practices to keep in mind:
- Timing and nudges: Send check-in prompts a few days before the visit, with a reminder closer to arrival. Using both text and email increases completion rates.
- Designing for completion: Keep it short, mobile-friendly and easy to navigate. Clear steps and a save-and-return option help prevent drop-off.
- Reducing friction with smart defaults: Pre-fill what you can and only ask for what’s necessary. Less typing makes a big difference.
- Handling common blockers: Make it easy to recover passwords, upload insurance and understand balances. Small issues can quickly lead to abandonment.
- Setting expectations: Be clear about what’s done and what happens next so patients know exactly what to expect when they arrive.
On-site check-in options: kiosks, tablets and front desk workflows
Even with strong pre-registration, not every patient will complete check-in ahead of time. That’s where on-site options come in. The goal is to create a flexible setup that keeps patients moving while giving staff clear ways to step in when needed.
Here are the options and factors to consider:
- When kiosks/tablets make sense: Kiosks and tablets are especially useful in higher-volume settings where front desks can become bottlenecks. They give patients a self-service option and help distribute check-ins more evenly across the space.
- Queue and arrival management: Clear arrival workflows—like digital check-in confirmations or queue tracking—help prevent crowding and confusion. Patients should know they’re in the system and what to expect next.
- Accessibility considerations: On-site check-in should work for everyone. That includes adjustable screen height, large readable text, multi-language options and clear prompts for assistance when needed.
- Privacy and environmental design: Physical setup matters. Screen protectors, thoughtful spacing and clear signage help patients feel comfortable entering personal information in a shared space.
- Clear handoffs to staff for edge cases: Some patients will still need help—whether it’s complex insurance issues or accessibility needs. Staff should have clear visibility into where patients are in the process so they can step in quickly without disrupting the overall flow.
Security, privacy and compliance considerations
Here’s what to keep in mind:
- Protect patient data throughout the workflow: Patient information should be protected at every step. That includes secure data handling practices, access controls and systems designed to minimize the risk of unauthorized access.
- Payment security expectations: Any system that collects payments should follow established security standards, including encryption and tokenization, to protect financial information. Separating payment data from clinical data can further reduce risk.
- Identity and consent integrity: Digital check-in systems should clearly capture patient identity and consent, with audit trails that show what was signed, when and by whom. This helps support both compliance and clinical documentation.
- Vendor due diligence checklist: Healthcare organizations should evaluate vendors carefully, including their security certifications, data protection practices and incident response plans. It’s important to understand who has access to data and how it’s managed.
- Minimize risk in integrations: When systems connect (like check-in tools and EHRs), data needs to flow accurately and securely. Strong validation rules, monitoring and error handling help prevent issues like mismatched or incomplete records.
Implementation playbook: how to roll out digital check-in
A thoughtful rollout reduces disruption, builds staff buy-in and increases the likelihood that digital check-in actually delivers the operational improvements it promises.
Here’s how to do it:
- Map your current workflow and define the future-state patient check-in procedure: Start by documenting how check-in works today, including where delays, errors or handoff issues occur. Then define what the ideal workflow should look like across pre-visit, arrival and post-check-in steps.
- Align teams early: Check-in touches multiple groups, including front office, clinical ops, billing, IT and compliance. Bringing these stakeholders in early helps avoid misalignment and ensures the new process works across teams.
- Pilot plan: Start with a smaller rollout, such as a single site or patient group. Define success criteria upfront (like completion rates or reduced check-in time) and gather feedback from both patients and staff.
- Training and scripts: Staff play a key role in adoption. Provide clear training, simple scripts for guiding patients and troubleshooting resources so teams feel confident using the new system.
- Iterate and scale: Use what you learn from the pilot to refine workflows, then expand gradually. Standardizing processes across locations helps ensure consistency while still allowing flexibility where needed.
Measuring success: KPIs and ROI for medical check-in
Improving medical check-in only matters if it delivers measurable results. The right metrics help you understand what’s working, where patients are dropping off and whether changes are actually improving operations and financial performance.
Here’s what to track:
- Adoption and completion metrics: Track how many patients complete check-in online before arrival, how often kiosks are used and where patients drop off in the process. These metrics gauge promise in your patient check-in system, says Moore.
- Time and throughput metrics: Look at average check-in time, how many patients can be processed per hour and overall wait times. These indicators help quantify whether changes are reducing bottlenecks and improving flow.
- Financial metrics: Measure point-of-service collections, payment plan uptake and denial rates tied to eligibility or data issues. Improvements here often signal that front-end workflows are supporting a stronger revenue cycle.
- Data quality metrics: Track registration error rates, duplicate records and missing information. Cleaner data at check-in reduces rework and downstream issues for both clinical and billing teams.
- Experience metrics: Use patient satisfaction scores, feedback themes and staff input to understand how the process feels on both sides, according to Moore. Adoption only sticks if the experience works for patients and staff alike.
The takeaway
- Medical check-in is a workflow, not a single step—and improving it can reduce friction across the entire patient journey.
- Shifting tasks before the visit helps reduce bottlenecks, improve data accuracy and ease pressure on front office staff.
- A well-designed patient check-in procedure supports faster patient flow, cleaner data and more reliable revenue cycle performance.
- The right medical check-in system should fit into existing workflows, offer flexible options for patients and provide clear visibility into performance.
- Successful implementation depends on more than healthcare technology—it requires workflow alignment, staff training and ongoing iteration.
Frequently asked questions (FAQs)
What is medical check-in in healthcare?
Medical check-in is the process of collecting and verifying key patient information before a visit. That includes demographics, insurance details, consent forms, payments and clinical questionnaires. It often starts before the appointment through digital tools and continues upon arrival to confirm everything is complete.
What’s the difference between a patient check-in procedure and a patient intake process?
A patient check-in procedure focuses on verifying and confirming information for a specific visit, like insurance, forms and payments. Patient intake is broader—it includes gathering clinical history, health information and financial details that may be used across multiple visits. Check-in is typically one step within the larger intake process.
How does a medical check-in system reduce wait times?
A medical check-in system reduces wait times by shifting tasks before the visit and streamlining what happens at arrival. When patients complete forms and verify information ahead of time, front desk staff can focus on exceptions instead of starting from scratch, which helps move patients through more quickly.
Are patient check-in kiosks worth it?
For many organizations, kiosks are worth it—especially in higher-volume settings. They provide a self-service option that can reduce front desk congestion and improve patient flow, while still allowing staff to step in when needed.
What features matter most when choosing a patient check-in system?
Key features include multi-channel check-in options (mobile, kiosk, staff-assisted), real-time insurance verification, flexible payment tools, pre-registration capabilities, reporting and analytics, and strong integration with existing EHR and practice management systems.
Conclusion
Medical check-in plays a bigger role than it’s often given credit for. When designed intentionally, it can streamline patient flow, improve data accuracy, support collections and reduce strain on staff.
The most effective approach is to treat check-in as a connected workflow, starting before the visit and carrying through arrival. Map your current patient check-in procedure, identify friction points and prioritize high-impact improvements. Then choose a medical check-in system that fits your workflows and implement it with clear goals and measurable outcomes.
The bottom line: When check-in works, everything downstream functions better.
A version of this article was originally published on February 13, 2022.